Restorative CNA: Duties, Training, Salary & How to Get Started
Learn what a restorative CNA does, how to get certified, expected salary, job duties, and training programs. Your complete guide to restorative nursing aide...
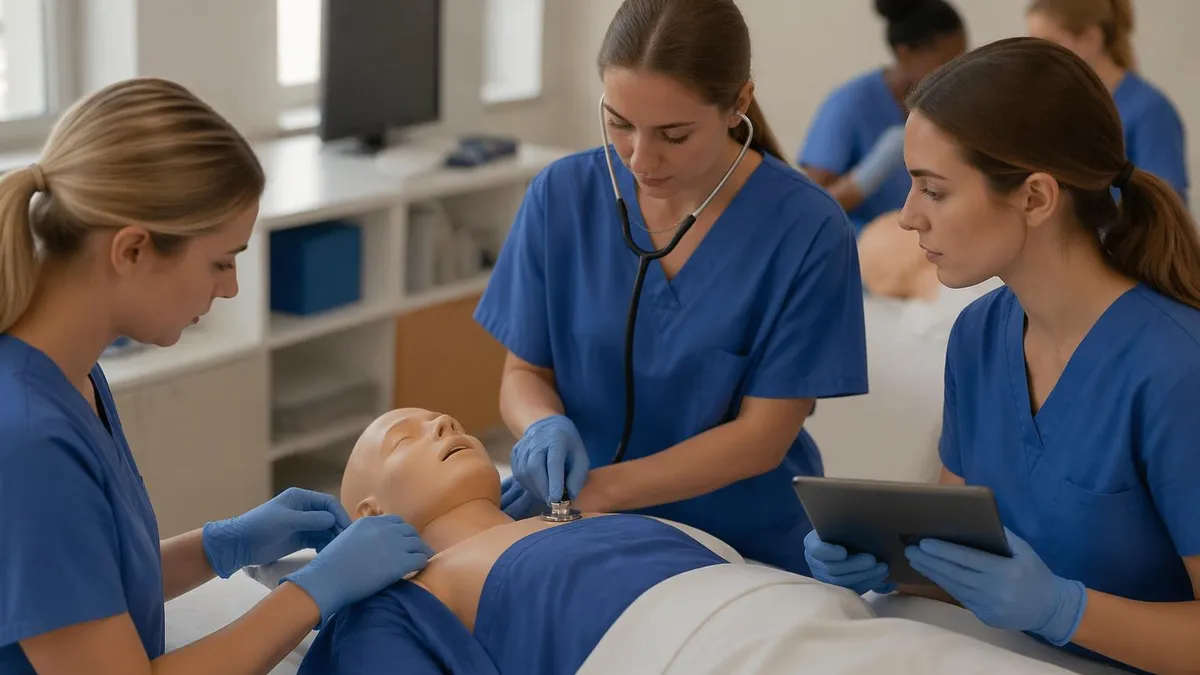
A restorative cna works in a specialized role that focuses on helping patients regain independence through targeted exercise programs, mobility training, and daily living skill rebuilding. Unlike standard CNAs who handle general patient care, restorative nursing aides design and carry out individualized care plans that emphasize rehabilitation over routine maintenance. If you're looking for restorative cna jobs, you'll find openings in skilled nursing facilities, rehabilitation centers, and long-term care homes across the country.
The demand for restorative CNAs keeps growing as the aging population expands and healthcare facilities shift toward outcome-based care models. Medicare and Medicaid reimbursement rules now tie funding to patient improvement metrics, which means facilities need staff who can document and deliver measurable progress. That's exactly what a restorative CNA does—bridge the gap between physical therapy sessions and everyday patient care by reinforcing exercises and tracking functional gains throughout the day.
Whether you're already a certified nursing assistant looking to specialize or you're exploring healthcare careers from scratch, the restorative path offers better pay, more autonomy, and a genuinely rewarding daily routine. You'll spend less time on custodial tasks and more time working one-on-one with patients who are actively trying to improve. It's a career niche that rewards patience, creativity, and genuine investment in people's recovery journeys. This guide covers everything from certification requirements and salary data to the specific duties you'll handle on a typical shift.
Restorative CNA Quick Stats
Finding restorative cna jobs isn't difficult once you have the right credentials. Most openings appear at skilled nursing facilities (SNFs), where Medicare regulations require dedicated restorative nursing programs. These facilities actively recruit CNAs who've completed restorative cna training because they need staff who understand range-of-motion exercises, ambulation techniques, and proper documentation of patient outcomes. Job boards like Indeed, LinkedIn, and specialized healthcare sites post hundreds of restorative CNA positions weekly.
Restorative cna training programs typically run four to twelve weeks on top of your standard CNA certification. Some employers offer in-house training—you get paid while learning the restorative skill set. Community colleges and vocational schools also run standalone programs, usually costing $200 to $800. The curriculum covers exercise physiology basics, restorative nursing techniques, patient motivation strategies, and regulatory documentation requirements that facilities need for Medicare compliance.
The job market favors candidates with both CNA certification and restorative training. Facilities that lose their restorative aide face compliance issues and potential Medicare reimbursement penalties, so retention tends to be stronger in these roles compared to general CNA positions. You'll also find that restorative positions are often Monday-through-Friday with regular daytime hours—a scheduling perk that's rare in bedside nursing aide work and one that makes the role especially attractive to experienced CNAs.
The restorative cna salary typically exceeds what general CNAs earn. National averages put restorative nursing aides at $38,000 to $48,000 annually, compared to $33,000–$40,000 for standard CNA roles. The premium reflects the specialized training and the direct impact these positions have on facility reimbursement rates. In high-cost-of-living areas—like California, New York, or Massachusetts—restorative CNAs can earn $50,000 or more with overtime and shift differentials factored in.
Restorative cna certification requirements vary by state, but the foundation is always the same: you need an active CNA license first. From there, restorative training adds specialized skills in therapeutic exercise programs, activities of daily living (ADL) retraining, splint and brace care, and cognitive stimulation techniques. Some states require a specific number of continuing education hours focused on restorative care, while others accept employer-provided training as sufficient qualification.
Career advancement from a restorative CNA position is straightforward. Many restorative aides move into restorative nursing coordinator roles, where they supervise other CNAs and manage the facility's entire restorative program. From there, some pursue LPN or RN licensure, using their restorative background as a springboard into physical therapy assistant programs or rehabilitation nursing specialties. The specialized experience makes your resume stand out in any healthcare setting.
Training & Certification
You'll need an active CNA certification before starting restorative training. Most states require completion of a state-approved CNA program (75–180 hours) and passing the NNAAP or state-specific competency exam. Once certified, you're eligible for restorative training programs. Some employers hire uncertified candidates and sponsor both CNA and restorative training simultaneously, though this is less common. A clean background check, current CPR/BLS certification, and TB test are standard requirements across all states.
What is a restorative cna, exactly? It's a certified nursing assistant who specializes in rehabilitation-focused care. While a standard CNA might help a patient get dressed and monitor vital signs, a restorative CNA actively works to improve that patient's ability to dress independently. The distinction matters—it's the difference between doing things for patients and teaching patients to do things for themselves. This philosophy shapes every aspect of the role, from how you interact with patients to how you document their progress.
Understanding the aging process and restorative care cna connection is critical to performing this job well. As people age, muscle mass decreases, joints stiffen, balance deteriorates, and cognitive function can decline. Restorative care directly addresses these changes through targeted interventions. Range-of-motion exercises maintain joint flexibility, strengthening programs slow muscle loss, balance training reduces fall risk, and cognitive activities preserve mental sharpness. You're essentially fighting against the natural decline that aging brings—and in many cases, you can reverse months or years of functional loss.
The psychological component is just as important as the physical one. Patients in long-term care often lose motivation when they feel like their independence is permanently gone. A skilled restorative CNA knows how to set achievable goals, celebrate small victories, and keep patients engaged in their own recovery. Sometimes the biggest breakthrough isn't a physical milestone—it's the moment a patient believes improvement is still possible after months of decline.
Daily Duties & Responsibilities
Lead individualized range-of-motion, strengthening, and balance exercises designed by the rehabilitation team. Track repetitions, resistance levels, and patient tolerance for each session to ensure steady progress toward care plan goals.
Coach patients through activities of daily living—dressing, grooming, eating, and toileting—using adaptive techniques and equipment. The goal is maximum independence, not task completion, so you teach rather than do.
Record patient progress on restorative nursing flow sheets and in the electronic health record. Accurate documentation supports Medicare reimbursement claims and helps the care team adjust treatment plans based on real outcomes.
Work with physical therapists, occupational therapists, nurses, and physicians to develop and update patient care plans. You're the daily eyes and ears—your observations shape the team's clinical decisions and discharge planning.
What does a restorative cna do on a typical shift? Your day starts with reviewing care plans and checking in with the nursing team about any overnight changes. Then you move through your patient caseload—typically six to ten residents—conducting individualized exercise sessions, ADL retraining, and mobility practice. Each session runs 15 to 30 minutes, and you document everything in real time. Between sessions, you might adjust exercise equipment, update flow sheets, or consult with the physical therapist about a patient's progress. Restorative cna duties are hands-on but intellectually engaging.
The specific tasks in your day depend on your patients' care plans. One resident might need range-of-motion exercises for stiff shoulders. Another might be practicing walking with a rollator after hip replacement surgery. A third could be relearning how to button a shirt following a stroke. You adapt your approach constantly—no two sessions look the same, and no two patients respond identically to the same intervention. Flexibility and creativity are essential traits for this role.
Afternoon shifts often include group activities—fall prevention classes, seated exercise groups, or cognitive stimulation sessions. These complement the one-on-one work and help build social connections among residents. You're also responsible for reporting any functional declines to the nursing staff, because a sudden drop in ability could signal a medical issue that needs immediate attention. The restorative CNA is often the first person to notice when something's wrong, precisely because you see each patient perform daily functional tasks.
Career Pros & Cons
- +Higher pay than standard CNA positions—typically $3–$5 more per hour
- +More predictable schedule with many positions offering Monday–Friday daytime hours
- +Greater autonomy and less direct supervision than bedside CNA roles
- +Deeply rewarding work watching patients regain independence
- +Strong job security due to Medicare compliance requirements at SNFs
- +Clear advancement path to coordinator, LPN, or RN roles
- −Requires additional training beyond standard CNA certification
- −Heavy documentation workload to meet Medicare requirements
- −Emotionally taxing when patients plateau or decline despite your efforts
- −Limited positions at smaller facilities that don't run restorative programs
- −Physical demands—you're on your feet assisting with exercises all shift
- −Some facilities understaff restorative programs, overloading remaining aides
A restorative cna job description typically lists several core competencies beyond basic CNA skills. Employers want candidates who understand therapeutic exercise principles, can demonstrate proper body mechanics during patient transfers, and have experience with documentation systems like PointClickCare or MatrixCare. Many job postings also mention patient motivation skills—facilities know that technical ability without interpersonal effectiveness won't produce the outcomes Medicare demands.
Restorative cna job duties span clinical, administrative, and interpersonal domains. On the clinical side, you're executing exercise programs, monitoring vital signs during activity, and assessing patients for pain or discomfort. Administratively, you're maintaining flow sheets, updating care plans, and contributing to quarterly MDS (Minimum Data Set) assessments. Interpersonally, you're encouraging reluctant patients, communicating with families about progress, and coordinating with therapists. It's a multifaceted role that challenges you differently every day.
The documentation piece deserves special emphasis. Medicare surveyors review restorative nursing records during facility inspections, and incomplete or inaccurate documentation can trigger deficiency citations. As a restorative CNA, your charting directly affects the facility's regulatory standing and reimbursement rates. Learning to write clear, objective, and timely notes isn't just a skill—it's a professional responsibility that carries real financial consequences for your employer and real care consequences for your patients.
Study Resources & CNA Test Prep
Restorative cna classes are available through community colleges, vocational schools, online platforms, and directly through employer-sponsored programs. The best programs combine classroom instruction with clinical practicum hours at a skilled nursing facility, giving you hands-on experience with real patients before you're working independently. Restorative cna meaning goes beyond a job title—it describes a philosophy of care that prioritizes patient independence and functional improvement over passive assistance. When you understand that philosophy, the clinical skills follow naturally.
The restorative cna job description you'll encounter in job postings varies by facility, but the core remains consistent across the industry. Most facilities want someone who can manage a caseload of six to ten patients, execute individualized exercise programs, maintain accurate documentation, and communicate effectively with the interdisciplinary care team. Some postings add specialized requirements like dementia care experience, wound care knowledge, or bilingual proficiency—these are bonus qualifications that can boost your starting pay.
Online courses have made restorative training more accessible than ever. Platforms like CareAcademy and Relias offer self-paced restorative nursing modules that some states accept for certification purposes. However, clinical hours are harder to replicate online, so most hybrid programs still require in-person practicum components. If you're in a rural area without nearby training programs, check whether your employer will sponsor on-the-job training—many facilities prefer this approach because they can tailor the training to their specific patient population and documentation systems.
Why Restorative CNA Roles Are Growing
Medicare's Patient-Driven Payment Model (PDPM) ties facility reimbursement to patient outcomes, not just services delivered. This means skilled nursing facilities need restorative CNAs who can demonstrate measurable patient improvement. Facilities without strong restorative programs risk lower reimbursement rates and regulatory citations. For CNAs, this creates a stable, well-paying career niche with growing demand through at least 2034.
Understanding cna chapter 9 rehabilitation and restorative care from your CNA textbook is the academic foundation, but the real learning happens on the floor. Chapter 9 covers the principles—promote independence, maintain function, prevent further decline—and the restorative skills cna test will assess whether you can apply those principles in clinical scenarios. Expect questions about range-of-motion exercises, proper body mechanics, ADL retraining techniques, and the role of the restorative aide within the care team hierarchy.
The restorative skills cna test format depends on your state and training program. Some programs use written exams with multiple-choice and scenario-based questions. Others include a clinical skills demonstration where you perform exercises and techniques on a mannequin or standardized patient. The best preparation combines studying theory with practicing hands-on skills—reading about passive range-of-motion is useful, but actually performing it on another person builds the muscle memory and confidence you'll need on the job.
Study groups with fellow CNA students can be incredibly effective for test prep. Pair up to practice ROM exercises on each other, quiz one another on terminology, and walk through care plan scenarios together. Many successful restorative CNAs say that peer practice was more valuable than any textbook chapter. The exam tests practical knowledge, not memorization—so focus your study time on understanding why you perform each technique, not just the steps involved. That deeper understanding will serve you well in interviews and on the job itself, where clinical reasoning matters far more than rote recall.
While all states require CNA certification as a baseline, restorative CNA requirements differ significantly. Some states mandate a specific restorative nursing training program with minimum hours, while others accept employer-provided on-the-job training. Before investing in a program, verify your state's requirements through your state nursing board website or by contacting a local skilled nursing facility's nursing education department.
Restorative care cna roles differ from general nursing aide positions in both scope and expectations. Where a standard CNA follows a task-based routine—vital signs, meals, bathing, toileting—a restorative care CNA follows a goal-based approach. Every interaction with a patient is an opportunity to reinforce independence. Helping someone with lunch? A restorative aide might use adaptive utensils and coach the patient through self-feeding rather than simply delivering a tray. That mindset shift is what separates the two roles.
The restorative aide vs cna debate often comes down to career goals and personality fit. If you prefer structured, predictable tasks with clear completion markers, standard CNA work might suit you better. If you thrive on problem-solving, enjoy tracking progress over weeks and months, and find motivation in patient breakthroughs, restorative care is your lane. The pay premium is a nice bonus, but most restorative CNAs cite job satisfaction—not salary—as the primary reason they chose the specialty.
Facilities increasingly recognize that restorative care reduces overall healthcare costs. Patients who maintain functional independence require fewer hospitalizations, less intensive nursing care, and shorter rehabilitation stays. A good restorative CNA program can save a facility hundreds of thousands of dollars annually in reduced hospital readmissions and improved survey outcomes. That financial reality is why restorative positions are among the most recession-proof roles in long-term care.
Cna restorative care is gaining recognition as a distinct healthcare discipline rather than just a CNA subspecialty. Professional organizations like the American Health Care Association (AHCA) and the National Association of Health Care Assistants (NAHCA) now offer dedicated restorative care tracks at their annual conferences. This professionalization benefits working restorative CNAs by establishing standardized competencies, creating networking opportunities, and advocating for better compensation across the industry.
If you're a cna restorative professional looking to stay current, join online communities and attend facility in-services whenever they're offered. The field evolves as research uncovers better rehabilitation techniques and technology introduces new tools—from wearable activity trackers that monitor patient movement to tablet-based cognitive exercise programs that engage patients between formal therapy sessions. Staying informed helps you deliver better care and positions you for advancement.
The future of cna restorative work looks strong. An aging Baby Boomer population, combined with healthcare's shift toward value-based reimbursement, ensures growing demand through at least the next decade. Facilities that invest in restorative programming see better patient outcomes, higher family satisfaction scores, and fewer regulatory deficiencies. For CNAs willing to invest in additional training, the restorative path offers a career with purpose, stability, and room to grow.
CNA Questions and Answers
About the Author
Registered Nurse & Healthcare Educator
Johns Hopkins University School of NursingDr. Sarah Mitchell is a board-certified registered nurse with over 15 years of clinical and academic experience. She completed her PhD in Nursing Science at Johns Hopkins University and has taught NCLEX preparation and clinical skills courses for nursing students across the United States. Her research focuses on evidence-based exam preparation strategies for healthcare certification candidates.