ACLS Subject Knowledge — What Every Provider Must Know for Certification
ACLS subject knowledge guide covering algorithms, pharmacology, rhythm recognition, and team leadership. Free practice tests to prepare for your ACLS exam.
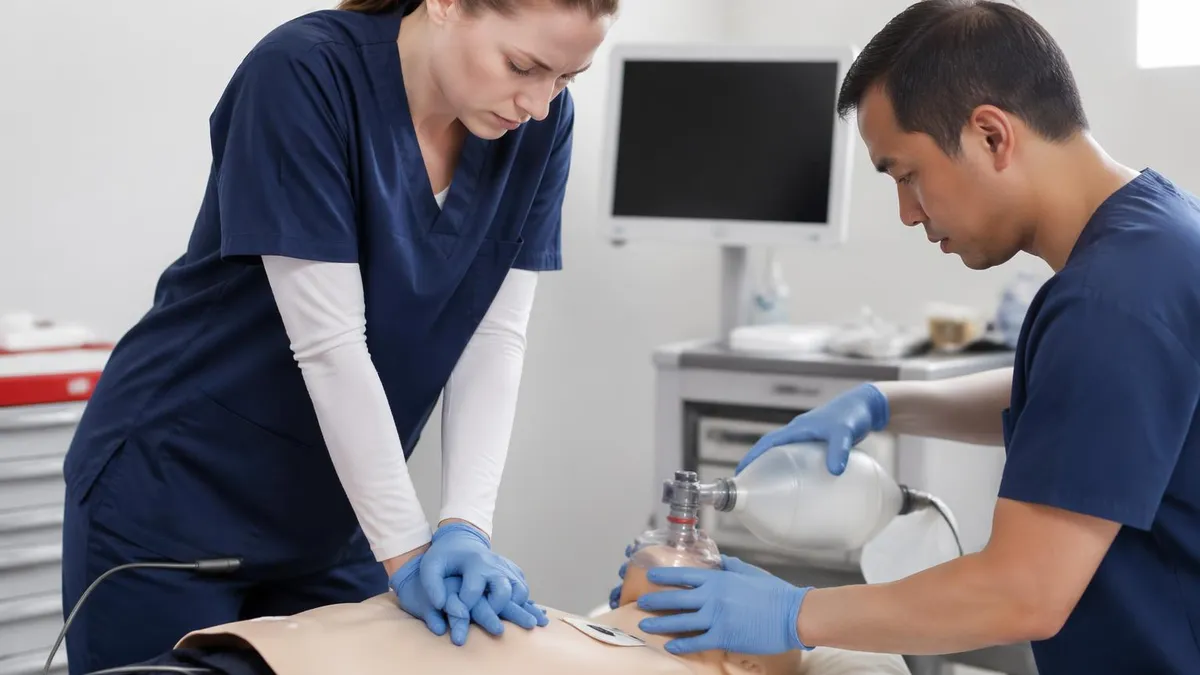
ACLS subject knowledge goes far beyond memorizing algorithms. It's the clinical reasoning that connects rhythm recognition to drug selection to electrical therapy — and the team dynamics that tie everything together under pressure. If you're preparing for ACLS certification, you need to understand not just what to do, but why each intervention matters and when to pivot between approaches.
One area that catches candidates off guard is knowledge sharing by a team leader ACLS — the structured communication patterns that keep a resuscitation team coordinated during cardiac arrest. An example of knowledge sharing by a team leader ACLS scenario: the leader verbalizes the current algorithm step, confirms drug administration, and redirects team members when priorities shift. It sounds simple on paper. But in actual practice, it's the skill that separates competent providers from effective ones.
This guide covers every major subject domain tested on the ACLS exam: cardiac arrest algorithms, pharmacology, rhythm interpretation, airway management, acute coronary syndromes, stroke protocols, and team leadership. Whether you're taking ACLS for the first time or renewing your certification, test your baseline with an ACLS Airway Management practice test before your course starts.
ACLS Exam at a Glance
Cardiac Arrest Algorithms — The Foundation of ACLS Knowledge
Everything in ACLS starts with the cardiac arrest algorithm. The first branch point: is the rhythm shockable or not? Ventricular fibrillation (VF) and pulseless ventricular tachycardia (pVT) are shockable — they respond to defibrillation. Pulseless electrical activity (PEA) and asystole are non-shockable — they require identifying and treating reversible causes. This distinction drives every subsequent decision. An example of knowledge sharing by a team leader ACLS involves the leader calling out which branch of the algorithm applies so the entire team knows the treatment pathway.
For shockable rhythms, the sequence is clear: defibrillate immediately, resume CPR for two minutes, check rhythm, repeat. Epinephrine enters after the second shock (1 mg IV every 3–5 minutes). Amiodarone comes after the third shock — 300 mg first dose, 150 mg second. Lidocaine is the alternative if amiodarone isn't available. Don't overthink the timing. Stick to the algorithm. It exists because structured approaches save more lives than improvisation.
Non-shockable rhythms are harder to manage because there's no definitive electrical fix. High-quality CPR and epinephrine are your primary tools. But the real work is identifying reversible causes — the Hs and Ts. Hypovolemia, hypoxia, hydrogen ion excess, hypo/hyperkalemia, and hypothermia. Tension pneumothorax, tamponade, toxins, and thrombosis. Exam questions on the Hs and Ts appear frequently, and an example of knowledge sharing by team leader ACLS expects leaders to verbalize which reversible causes they're considering in real time.
ACLS Pharmacology — Drugs You Must Know Cold
Pharmacology trips up more ACLS candidates than any other subject area. Not because the drugs are complicated — they aren't. Because the dosing, timing, and indications must be automatic. There's no time to look things up during a code. Example of knowledge sharing by team leader ACLS: the leader orders "epinephrine 1 mg IV push" and the medication nurse repeats the order back before administering. That closed-loop pattern prevents errors when stress runs high.
Epinephrine is the workhorse. One milligram IV push every 3–5 minutes in cardiac arrest — regardless of rhythm. For symptomatic bradycardia, it's an infusion at 2–10 mcg/min. Amiodarone treats refractory VF/pVT: 300 mg IV bolus first, then 150 mg if needed. Atropine handles symptomatic bradycardia at 0.5 mg IV, repeatable every 3–5 minutes up to 3 mg total. Adenosine converts stable narrow-complex SVT: 6 mg rapid IV push, then 12 mg if the first dose fails.
Here's where candidates stumble: contraindications. Atropine doesn't work for second-degree type II or third-degree heart block — those patients need pacing. Adenosine requires a rapid push followed by a flush because its half-life is under 10 seconds. Amiodarone can cause hypotension, so monitor blood pressure post-administration. These details appear on the written exam and in skills stations. Know them backward and forward before your course date.
ACLS Algorithm Quick Reference
Shockable (VF/pVT): Defibrillate → CPR 2 min → check rhythm → repeat. Epinephrine 1 mg IV after 2nd shock, then every 3–5 min. Amiodarone 300 mg after 3rd shock, then 150 mg. Non-shockable (PEA/Asystole): CPR → Epinephrine 1 mg IV every 3–5 min → identify reversible causes (Hs and Ts). No defibrillation. Continue high-quality CPR with minimal interruptions.
Rhythm Recognition — Reading ECG Strips Under Pressure
You can know every algorithm perfectly and still fail ACLS if you can't read the rhythm. It's that important. The written exam shows you ECG strips. The skills stations show you live monitors. In both cases, you need to identify the rhythm within seconds — not minutes. Knowledge sharing by team leader ACLS demands that the leader announce the identified rhythm to the team before directing interventions.
Start with the lethal rhythms. VF looks chaotic — no organized complexes, no discernible pattern, just electrical noise. pVT shows wide, regular complexes at a fast rate with no discernible P waves. Asystole is a flat line (confirm by checking leads and gain). PEA looks like any organized rhythm on the monitor, but the patient has no pulse — that's the catch. You have to check the patient, not just the screen.
Then learn the non-lethal rhythms that still require intervention. Sinus bradycardia is slow but organized. SVT (supraventricular tachycardia) is fast and narrow. Atrial fibrillation shows irregularly irregular R-R intervals. Second-degree type II block has dropped QRS complexes without progressive PR prolongation. Third-degree block shows complete AV dissociation. Each rhythm maps to a specific algorithm branch. If you misidentify the rhythm, you'll follow the wrong treatment path — and on the exam, that's a fail. Practice with real rhythm strips until identification becomes reflexive. Speed matters here more than anywhere else in ACLS.
Core ACLS Subject Areas Tested
Shockable vs. non-shockable rhythms, high-quality CPR standards, defibrillation protocols, and the Hs and Ts framework for identifying reversible causes during active codes.
Epinephrine, amiodarone, atropine, adenosine, lidocaine — correct dosages, timing, routes of administration, contraindications, and the closed-loop verification process.
Basic and advanced airway interventions including bag-valve-mask ventilation, supraglottic airways, endotracheal intubation, waveform capnography, and ventilation rates during CPR.
Closed-loop communication, role assignment, constructive intervention, mutual respect, and knowledge sharing between team leader and members during high-stress resuscitation scenarios.
Team Dynamics — Why Knowledge Sharing by Team Leader ACLS Matters
ACLS isn't a solo performance. Every cardiac arrest response involves multiple providers working simultaneously — someone does compressions, someone manages the airway, someone pushes drugs, someone monitors the rhythm. The team leader coordinates all of it. And the single most tested team skill on the ACLS exam? Knowledge sharing by team leader ACLS — the practice of verbalizing your clinical reasoning so everyone on the team understands the plan.
Here's what that looks like in practice. The team leader identifies the rhythm: "I'm seeing VF — we're following the shockable arrest algorithm." Clear. Specific. Now everyone knows the treatment pathway. After the shock: "Resume compressions. Prepare epinephrine 1 mg IV — we'll give it after this cycle." The medication nurse repeats: "Epinephrine 1 mg IV, preparing now." That's closed-loop communication. The AHA tests this explicitly.
Candidates who treat the team dynamics component as filler content fail at higher rates. The AHA has emphasized team-based resuscitation since the 2010 guideline update, and it shows up in every skills station. You'll be evaluated as both team leader and team member. As a member, your job is to speak up if you see something wrong — constructive intervention. As the leader, your job is to share knowledge continuously so no one is guessing what comes next.
Pros and Cons of ACLS Certification
- +Required credential for most acute care nursing, physician, and PA positions
- +Structured AHA curriculum with clearly defined testable content areas
- +Two-year certification cycle — renewal is shorter and faster than initial course
- +Blended learning format lets you complete theory online at your own pace
- +Skills translate directly to real clinical practice — not just academic exercise
- +Multiple preparation resources available at every budget level
- −BLS prerequisite adds an extra certification step before you can start ACLS
- −Most hospitals only accept AHA certification — third-party online providers may not qualify
- −84% passing score is relatively high compared to many other healthcare exams
- −Skills stations test real-time decision making — harder to prepare for than written content
- −Course costs range from $150–$350 and aren't always reimbursed by employers
- −Letting certification lapse more than 90 days means retaking the full initial course
ACS and Stroke Protocols — Time-Critical ACLS Knowledge
Acute coronary syndromes and stroke are two ACLS subject areas where time literally equals tissue. For ACS, the clock starts at first medical contact. A 12-lead ECG within 10 minutes is mandatory. Aspirin (160–325 mg chewed) goes in immediately unless contraindicated. Nitroglycerin addresses ongoing chest pain. Oxygen only if SpO2 drops below 90%. Knowledge sharing by team leader ACLS in ACS scenarios involves communicating the ECG findings and activating the catheterization lab for STEMI patients without delay.
The stroke algorithm follows the Cincinnati Stroke Scale — facial droop, arm drift, and speech abnormality. Any positive finding triggers an immediate CT scan. The critical decision: is this ischemic or hemorrhagic? Ischemic stroke patients may qualify for tPA (alteplase) if they're within 3 to 4.5 hours of symptom onset and meet eligibility criteria. Hemorrhagic stroke is a tPA contraindication. Getting the timeline wrong — or missing the window — has devastating consequences for the patient.
Both protocols test your ability to act fast while following a structured approach. The ACLS exam presents these as scenario-based questions where you'll need to sequence interventions correctly. Know the time benchmarks: door-to-ECG in 10 minutes for ACS, door-to-CT in 25 minutes for stroke, door-to-needle in 60 minutes for tPA. These numbers appear consistently on the written exam and in skills stations.
ACLS Written Exam Preparation Checklist
Airway Management — Advanced Interventions in ACLS
Airway management is one of the first hands-on skills tested in ACLS. It starts simple — bag-valve-mask (BVM) ventilation with proper head-tilt chin-lift positioning. But it escalates quickly into advanced techniques. Supraglottic airways (like the King LT or i-gel) provide a secondary option when BVM ventilation isn't adequate. Endotracheal intubation remains the gold standard for definitive airway control, though it requires practice and shouldn't interrupt chest compressions for more than 10 seconds.
Waveform capnography is the confirmation method you need to know. After placing an advanced airway, capnography confirms correct tube placement and monitors CPR quality. A sudden spike in end-tidal CO2 during a code often indicates return of spontaneous circulation (ROSC) — that's a good sign. Knowledge sharing by team leader ACLS includes announcing capnography readings so the team can assess resuscitation effectiveness in real time.
Ventilation rates matter more than most candidates realize. During CPR without an advanced airway: 30 compressions to 2 breaths. With an advanced airway in place: continuous compressions at 100–120 per minute with one breath every 6 seconds (10 breaths per minute). Hyperventilation is a common and dangerous mistake — it increases intrathoracic pressure, reduces venous return, and decreases coronary perfusion. The exam tests this explicitly, and skills evaluators watch for it closely.
Focus on Decision Points, Not Just Steps
The ACLS exam doesn't just test whether you know the algorithm steps — it tests whether you can make the right decision at each branch point. Is the rhythm shockable or not? Is the patient stable or unstable? Is the QRS narrow or wide? Practice identifying these decision points first, then work through the interventions that follow each branch. This approach mirrors how real resuscitations unfold and matches the way AHA scenario-based questions are structured.
Post-Cardiac Arrest Care — The Final ACLS Subject Domain
Surviving cardiac arrest doesn't end with ROSC. Post-cardiac arrest care is a distinct ACLS subject area covering the critical interventions needed in the first 24–48 hours. Targeted temperature management (TTM) — cooling the patient to 32–36°C for at least 24 hours — is the headline intervention. It improves neurological outcomes in patients who remain comatose after ROSC. Knowledge sharing by team leader ACLS continues in this phase, with the leader communicating temperature targets and hemodynamic goals to the ICU team.
Hemodynamic optimization matters immediately after ROSC and can't wait for the ICU transfer. The target: systolic blood pressure above 90 mmHg, or a mean arterial pressure above 65 mmHg. Vasopressors and IV fluids achieve this. A 12-lead ECG post-ROSC identifies any ST-elevation that warrants emergent catheterization. Blood glucose management, seizure prevention, and avoiding hyperoxia (keeping SpO2 between 92–98%) round out the post-arrest protocol.
This subject area appears less frequently on the written exam than cardiac arrest algorithms, but it shows up. Candidates who skip post-arrest care in their study plan leave easy points on the table. It's also increasingly emphasized in renewal courses as the AHA updates its guidelines to reflect growing evidence about post-ROSC interventions and neurological prognostication.
You cannot enroll in or complete ACLS certification without a current AHA BLS for Healthcare Providers card. If your BLS is expired, obtain BLS certification first. Most ACLS course providers verify BLS status before allowing you to participate. Both BLS and ACLS follow the same two-year renewal cycle — consider scheduling renewals together to keep both current simultaneously.
How to Prepare for the ACLS Written Exam
The AHA ACLS written exam has 50 questions. You need 84% or higher to pass — that means you can miss no more than 8 questions. The exam covers algorithms, pharmacology, rhythm recognition, and team dynamics. Most questions are scenario-based: you're presented with a clinical situation and asked to choose the correct next intervention. Knowledge sharing by team leader ACLS appears in questions about communication protocols and team management.
Start with the algorithms. Know the decision points cold. Then layer in pharmacology — which drug, what dose, when in the algorithm. Rhythm recognition is best practiced with actual ECG strips, not just textbook descriptions. Flashcards help for drug dosing. Practice tests help for everything else. Take at least three full-length practice exams before your course. Each one exposes gaps you didn't know existed. Focus extra time on whichever subject area gives you the most trouble — that's almost always either pharmacology dosing or rhythm identification under time pressure.
If you fail the written exam, you get one chance to remediate and retest during the same course session. If that second attempt fails, you'll need to retake the entire ACLS course from scratch — paying full tuition again. That's reason enough to prepare thoroughly. Use ACLS Cardiac Rhythm Recognition questions to drill the rhythm identification skills that trip up the most candidates on exam day.
ACLS Renewal — Keeping Your Subject Knowledge Current
ACLS certification lasts two years. Renewal is shorter than the initial course — typically 4–8 hours depending on format. The renewal exam and skills stations cover the same content, but the course assumes you already have foundational knowledge sharing by team leader ACLS experience and focuses on updates, refreshers, and areas where providers commonly lose proficiency between certification cycles.
AHA guidelines update every five years. The most recent major update was 2020, with the next expected in 2025. When guidelines change, renewal courses incorporate the new recommendations. Recent emphasis areas include minimizing compression interruptions, optimizing epinephrine timing in cardiac arrest, and expanding the focus on post-cardiac arrest care and targeted temperature management.
Schedule your renewal 30–60 days before expiration. Seats fill up — especially at hospital-based training sites. If your certification lapses by more than 90 days, most providers require you to retake the full initial course. That's significantly more time, more money, and more hassle than simply scheduling your renewal on time. Many hospitals track expiration dates for their staff, but the responsibility is yours. Check your employer's reimbursement policy before paying out of pocket — some facilities cover renewal costs for employed providers.
ACLS Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.